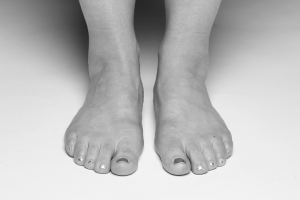
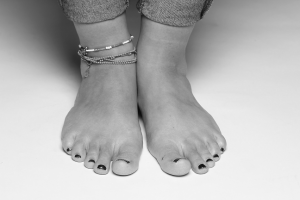
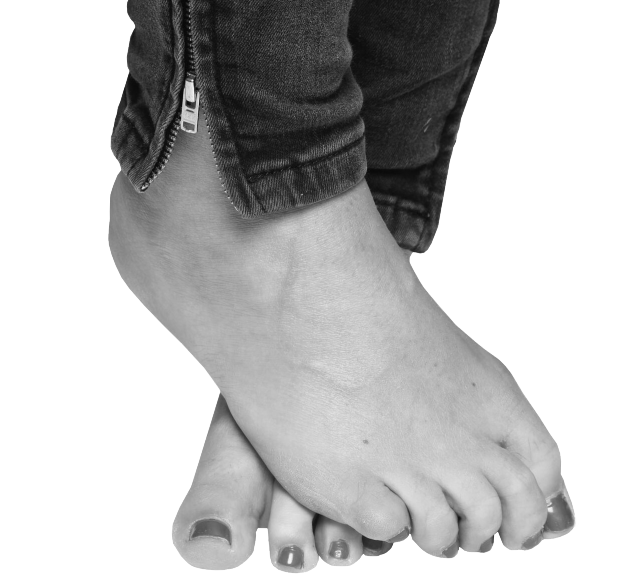
Common Foot Conditions
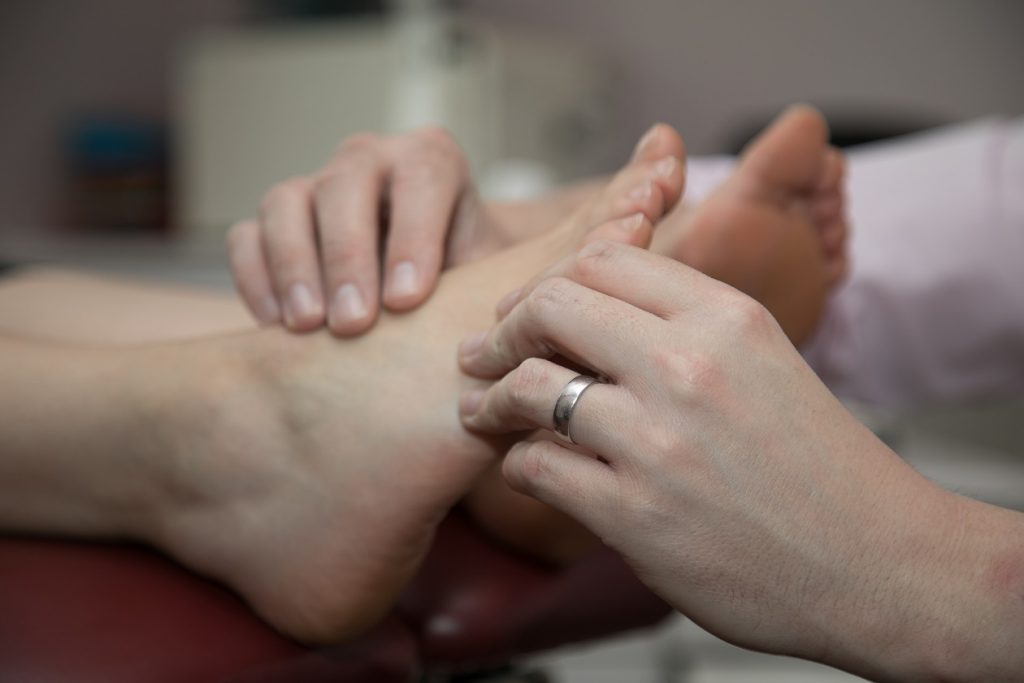

Corns are caused by abnormal pressure and friction known as mechanical stress. As a result of undue pressure and mechanical stress the skin builds a protective skin layer. This layer will become increasingly thickened and hard resulting in a hard corn or soft and rubbery resulting in a soft corn. The centre of the corn becomes compacted into a plug that penetrates into the skin.
Types of Corns:
- Hard Corn. Usually located on the top of the toes or on the sole of the foot.
- Soft Corn. Located between the toes where it remains constantly moist.
- Vascular or Neurovascular Corn. Mostly found on the sole of the foot, where blood vessels and nerves are forced into the corn by excessive pressure
- Seed Corns are hard beads of fat that form on the sole of the foot.
Home Treatment:
Although widely available corn plasters/preparations should be used with caution as they generally contain Salicylic Acid which is unsuitable for use by Diabetics, elderly, Children under 15, or people with poor circulation. It should also be noted that unfortunately people aren’t always aware that the prescription drugs they may take for one condition can cause a reduction of blood to the extremities having an adverse affect on the skin; meaning that most people do not realise that the medication they are taking can affect their circulation, and that the restrictions mentioned on the medicated corn plaster containers actually refer to them. Additionally there have been cases where medicated corn plasters that contain caustics designed to breakdown tissue have accidently moved; burning healthy skin resulting in severe inflammation, sepsis and ulceration developing on the corn site.
Appointment Treatments:
The Foot Health Practitioner can remove corns painlessly and safely and if the cause of the corn is removed, i.e. shoe pressure or the feet realigned by Orthotic Therapy, then it MAY be possible to eradicate the corns permanently.
Fungal nail infection is a very common problem, affecting around three in every 100 people in the UK. Around half of all nail problems are due to a fungal infection.
Fungal nail infection can look ugly because the nail often becomes thickened and discoloured. The nail can turn white, black, yellow or green. The nail can sometimes become brittle, with pieces of nail breaking off or even coming away from the toe completely.
Underneath and around the nail (the nailbed), the skin can sometimes become inflamed and painful. If a toenail is infected and painful, it can become difficult to walk.
Athlete’s foot
Fungal nail infection in the toenail is most commonly caused by a fungal skin infection, such as athlete’s foot. Around a third of people with athlete’s foot will also have a nail infection. Athlete’s foot usually affects the skin in between your toes, causing it to be red, flaky and itchy.
-Continually wearing sweaty/damp footwear (Fungi grow easily in warm, damp environments)
-Nail damage
-Having a health condition such as diabetes or psoriasis
-Being immunosuppressed (having a weakened immune system) or being in poor general health
-Living or working in a warm and humid climate
-Smoking
-Nail infections are more likely to happen with increasing age. Sometimes, there is no apparent cause for an infection. Treatments
-Antifungal tablets (prescribed by your GP)
-Topical antifungal nail paints/sprays or skin creams (available through your Foot Health Practitioner or Chemist).
Whichever method of treatment you choose, diligence on behalf of the patient is vital when treating fungal infections.
Stopping treatments too early can mean that the infection comes back.
*It should be noted that success with topical medications can take up to twelve months depending on the servery of the infection.*
An ingrown toenail is an extremely painful condition. It occurs when the edge of a nail penetrates the surrounding soft tissues of the toe; causing swelling, inflammation and infection. Ingrown toenails are commonly caused by poorly fitting shoes, but they can also be caused by improper trimming or by trauma.
Sometimes shoe pressure on the nail wall can result in callous (hard skin formation) in the nail groove and if left untreated this can build up and cause inflammation and infection, this condition is often mistaken and people believe they have an ingrown toenail.
The initial treatment of ingrown toe nails is based on conservative management. This involves the removal the offending nail splinter and dressing of the toe. Appointments are made to review the situation and ensure the nail does not penetrate the nail wall upon re-growth. Frequently ingrown toenails can be persistent and troublesome. In such cases nail surgery is recommended.
Verrucae are caused by a virus known as the human papilloma virus (HPV).
Verrucae may occur as single or multiple growths affecting any aspect of the feet. There is a considerable variation in the appearance of verrucae. Those on the sole of the feet may have their appearance modified by the weight of the body, which forces the verrucae’s mass into the foot giving them a flattened look, over which can be hard callous. For this reason verrucae may be mistaken for corns or hard skin. Other verrucae, e.g. Mosaic verrucae, tend to be shallow and pain-free, whilst the deep plantar verrucae, depending on their location, can be extremely painful.
Verrucae are contagious but the risk of catching them is relatively low. The virus can often gain entry into the skin during barefoot activities such as swimming, showering, trying on shoes in shoe shops without wearing hosiery, hotel rooms, saunas, gymnasiums or health farms. It is also recognised that stress and compromised immune systems are also a factor.
Unfortunately, if you are unlucky and do catch one, there is no proven effective treatment that works in every case. Some treatments work for some people whilst for others it will have no effect. The good news is that most verrucae will just disappear of their own accord with no treatment – although this may take up to 2 years, which is the verrucae’s usual life-span.
How To Treat
There are arguments to suggest that often the best treatment is to leave the verrucae alone to clear up itself. However if it is painful and/or is limiting what you can do then you may wish to try to treat.
If you do purchase any over the counter treatments, always read the information sheet to ensure it is suitable for you to use. If you have any concerns, always seek medical help.
Diabetics – You should never try to treat a verrucae yourself ALWAYS seek the advice of your GP, Diabetic Nurse or a qualified Foot Health Practitioner or Podiatrist.
Home Remedies (medically unproven – they may work for you but they may not.)
Duct tape – You soak your foot in warm water and then file the verrucae with an emery board, apply silver heavy-duty duct tape, leave on for 1 week, remove the tape, soak and file again. Leave open overnight, soak and file again as before, re-apply duct tape, leave on again for 1 week. Repeat this until it has gone.
Treatments performed by medical practitioners:
Dry Needling
Cryotherapy
Surgery
Low Intensity Laser Therapy (LILT)
Best thing to do is book an appointment to discuss your options.